When you or someone you care about is seriously ill, hospital terms can feel confusing. Two phrases often heard are ICU beds and critical care beds. Many people think they mean the same thing, but in hospitals, these terms have different meanings. Understanding the difference can make a big impact when you need to decide about care for yourself or a loved one.
Both types of beds are for patients who need close attention and advanced treatment. But the kind of care, equipment, and staff available can be quite different. These differences affect recovery, safety, and the resources a hospital uses. Sometimes, confusion about these terms leads to misunderstandings between doctors and families, or even between hospitals and the public.
In this article, you will learn the real differences between ICU beds and critical care beds. We’ll look at the history of these terms, key features, equipment, staff, patient types, and common myths. You’ll also find practical tips for families navigating the hospital system.
By the end, you’ll know exactly what questions to ask if you ever face these terms during a medical emergency.
What Is An Icu Bed?
The term ICU bed refers to a hospital bed located in an Intensive Care Unit (ICU). An ICU is a special area in a hospital for patients who are very sick or have life-threatening conditions. These units have advanced machines and highly trained staff. The main goal is to watch patients closely and react fast if their condition changes.
ICU beds are not just regular beds. They are designed with features to help doctors and nurses care for very sick patients. These beds can change position easily, help prevent bedsores, and support medical devices like ventilators and infusion pumps.
Most ICU beds are placed in rooms with glass walls, so staff can always see the patient.
One important thing: not every hospital uses the same standards for ICU beds. In some places, an ICU bed means full access to all ICU equipment and doctors. In other countries or smaller hospitals, an ICU bed might mean something less advanced. This difference matters when comparing hospitals or health systems.
What Is A Critical Care Bed?
A critical care bed is a broader term. It includes any hospital bed used for patients who need more attention and treatment than a regular hospital bed can give. That includes ICU beds, but also beds in other units, such as:
- High Dependency Units (HDUs): For patients who are very ill but not sick enough for ICU.
- Coronary Care Units (CCUs): For patients with serious heart problems.
- Surgical Intensive Care Units (SICUs): For patients after major surgery.
- Pediatric or Neonatal Intensive Care Units (PICUs/NICUs): For very sick children or newborns.
So, every ICU bed is a critical care bed, but not every critical care bed is an ICU bed. Critical care beds cover a range of care levels, from very close monitoring to just a little extra support. This is where confusion often begins.
Key Differences Between Icu Beds And Critical Care Beds
Understanding the differences requires looking at several factors: equipment, staff, patient type, and care level. Here’s how they compare.
| Feature | ICU Bed | Critical Care Bed |
|---|---|---|
| Location | Always in Intensive Care Unit | In ICU, HDU, CCU, or specialized care units |
| Staffing | Highest nurse-to-patient ratio (often 1:1 or 1:2) | Lower ratio (1:3 or 1:4), varies by unit |
| Equipment | Advanced life support, full monitoring | Some advanced tools, but not always full life support |
| Patient Type | Most critical, unstable, multi-organ support | Serious but more stable, single organ support |
| Level of Monitoring | Continuous, minute-by-minute | Frequent, but not always continuous |
Equipment And Technology
ICU beds have the most advanced technology in the hospital. Each bed usually has:
- Ventilators for patients who cannot breathe alone
- Cardiac monitors for real-time heart data
- Infusion pumps for controlled delivery of drugs or fluids
- Defibrillators in case of cardiac arrest
- Special mattresses to prevent pressure sores
Critical care beds outside the ICU may have some, but not all, of these. For example, an HDU bed may have cardiac monitoring and access to oxygen, but not a ventilator. Some units, like the CCU, focus more on heart monitoring than on full-body support.
Staffing And Training
A key difference is the staff-to-patient ratio. In ICUs, there is almost always one nurse for every one or two patients. These nurses have special training in critical care. Doctors, called intensivists, are present or nearby 24/7.
In other critical care units, the ratio is lower. One nurse may care for three or four patients. The doctors may not have the same level of critical care training and may not be present at all times.
Level Of Care
ICU beds are for patients who need the most help to stay alive. They may need support for more than one organ system (like heart and lungs). These patients can get worse very quickly, so they need constant monitoring.
Critical care beds outside the ICU are for patients who are less unstable. They still need frequent checks, but the risk of sudden changes is lower. For example, a patient recovering from major surgery may need a critical care bed for a day or two, but not full ICU care.
How Hospitals Decide Where A Patient Goes
Doctors use clear criteria to decide if someone needs an ICU bed or another critical care bed. These criteria include:
- Severity of Illness: Patients with life-threatening problems (like shock, severe infections, or major injuries) go to the ICU.
- Organ Support Needs: If a patient needs machines to help them breathe, filter their blood, or support their heart, they need an ICU bed.
- Risk of Deterioration: If doctors think a patient could get worse very quickly, they put them in the ICU.
- Type of Monitoring Required: If a patient only needs close observation or single organ support, a critical care bed in the HDU or CCU may be enough.
Hospitals often use scoring systems to help make these decisions. For example, the APACHE II or SOFA score helps doctors rate how sick a patient is. These scores help avoid mistakes, like putting a stable patient in the ICU or missing someone who really needs it.
Types Of Critical Care Beds (including Icu)
Let’s look at the main types of critical care beds and who uses them.
1. Intensive Care Unit (icu) Beds
These are for the sickest patients. Common reasons for ICU admission include:
- Severe pneumonia or sepsis
- Heart attacks with complications
- Major trauma (accidents)
- Multi-organ failure
- After certain major surgeries
ICU beds are always staffed and equipped for emergencies. These beds often have privacy curtains or glass walls, but open access for staff.
2. High Dependency Unit (hdu) Beds
An HDU is for patients who are very ill, but not as unstable as ICU patients. For example:
- After big surgeries, when the risk of problems is high
- Patients who have improved in the ICU but still need close watching
- Severe asthma attacks needing frequent treatments
HDUs have more monitoring and staff than regular wards, but less than the ICU.
3. Coronary Care Unit (ccu) Beds
A CCU is for heart problems. These beds are for:
- Heart attacks
- Dangerous heart rhythms
- Severe chest pain needing constant monitoring
CCUs have special equipment for heart monitoring and defibrillation.
4. Surgical Intensive Care Unit (sicu) Beds
SICU beds are for patients after major surgery who have a high risk of complications. These might include:
- Organ transplants
- Complicated abdominal surgeries
- Major vascular (blood vessel) operations
SICUs have equipment for monitoring and supporting many organ systems.
5. Pediatric And Neonatal Intensive Care Beds (picu/nicu)
PICUs are for critically ill children. NICUs are for newborn babies who are premature or very sick. These beds are smaller and have special equipment for infants, like incubators and pediatric ventilators.
The Role Of Bed Features And Design
You might think an ICU bed is just a regular hospital bed in a special room. In fact, the bed itself is highly specialized. Key features include:
- Adjustable positions: To help with breathing or prevent bedsores
- Built-in scales: To weigh patients without moving them
- Easy access for tubes and lines: For IVs, catheters, and monitors
- Alarms and controls: For quick adjustment by staff
Critical care beds in other units may not have all these features. For example, an HDU bed may have some adjustments, but not a built-in weighing scale. These details matter for patient safety and comfort.

Who Needs An Icu Bed Vs. A Critical Care Bed?
Patients who need an ICU bed often have:
- Sudden organ failure (heart, lungs, kidneys)
- Need for life support (ventilator, dialysis)
- Massive trauma or bleeding
- Unstable blood pressure needing strong medicines
Patients who need a critical care bed (but not ICU) often have:
- Recovering after major surgery, but stable
- Serious infections, but not in shock
- Heart problems needing close monitoring, not full life support
A common mistake: families often think a loved one must be in the ICU to get “proper” care. In reality, many patients recover just as well in an HDU or CCU if their condition allows.
Staffing: Training And Ratios Matter
The staffing of an ICU is one of its biggest strengths. Here’s a typical breakdown:
- Intensivists: Doctors trained in critical care medicine
- Critical care nurses: Special training, often 1 nurse per patient
- Respiratory therapists: For patients on breathing machines
- Pharmacists, physiotherapists, dietitians: Available for the sickest patients
In other critical care units, staff may have less training or cover more patients. For example, in an HDU, one nurse may care for three or four patients. The doctor may be a general physician, not a critical care specialist.
This difference in staffing can affect response times in emergencies. In the ICU, help is seconds away. In an HDU, it may take a few minutes longer. This is why truly unstable patients are always kept in the ICU.
Monitoring And Alarms: Constant Vs. Frequent
ICU beds have continuous, real-time monitoring for:
- Heart rate
- Blood pressure (sometimes with an internal line)
- Oxygen levels
- Breathing rate
- Urine output
If anything changes, alarms sound, and staff respond instantly.
In other critical care beds, monitoring is frequent but not always continuous. For example, vital signs may be checked every 15-30 minutes, or every hour. Alarms may alert staff, but the response may take a little longer.
This small difference can be critical for unstable patients, but for stable patients, it prevents unnecessary alarms and lets them rest.
Equipment: Full Life Support Vs. Partial Support
ICU beds are surrounded by machines:
- Mechanical ventilators: For patients who can’t breathe alone
- Hemodialysis machines: For kidney failure
- Multiple infusion pumps: For precise drug delivery
- Suction devices: To clear airways
- Defibrillators: Always nearby
In other critical care beds, not all this equipment is available. For example, a CCU may have heart monitors and defibrillators but not ventilators. An HDU may have access to oxygen and some pumps, but not dialysis.
This is why some patients are moved from one unit to another if their needs change.
Infection Control And Isolation
ICUs often have the strictest rules to prevent infection. This includes:
- Limited visitors
- Mandatory hand washing
- Special air filtration systems
- Private or semi-private rooms
Critical care beds in other units may have fewer isolation features. For example, in an HDU, there may be four patients in one room. This increases the risk of infection, so ICU is preferred for patients with weak immune systems.
Cost And Resource Use
ICU care is expensive. In developed countries, one day in the ICU can cost $3,000 to $10,000 or more, depending on care level and country. This is due to:
- Specialized staff
- Expensive equipment
- Intensive monitoring
Critical care beds outside the ICU cost less, as they use fewer resources and need less specialized staff. This is one reason why hospitals avoid keeping stable patients in the ICU longer than needed.

Common Myths And Misunderstandings
Many families and even some healthcare workers confuse these terms. Here are some myths:
- Myth: “Critical care bed” and “ICU bed” are the same.
- Reality: All ICU beds are critical care beds, but not all critical care beds are in the ICU.
- Myth: Patients recover better in the ICU.
- Reality: Stable patients may do better outside ICU, where there is less noise and risk of infection.
- Myth: Moving a patient from ICU to HDU means they are not getting proper care.
- Reality: It usually means the patient is improving and no longer needs full ICU support.
Understanding these facts can reduce stress and help you make better decisions.
Real-world Examples
Let’s consider two patients:
- Patient A: Admitted after a car accident, with lung and kidney failure. Needs a ventilator and dialysis. This patient needs an ICU bed.
- Patient B: Had major surgery, is stable but needs oxygen and close observation. This patient needs a critical care bed in the HDU.
If Patient B were kept in the ICU, they’d take up resources another, sicker patient might need.
Why Hospitals Track These Beds Separately
Hospitals and health systems keep separate counts of ICU beds and all critical care beds. This is important for planning, especially during emergencies like the COVID-19 pandemic. Knowing how many ICU beds are available helps hospitals direct the sickest patients to the right place.
For example, during COVID-19, many countries reported ICU bed capacity as a measure of readiness. But some also counted HDU and CCU beds to show how many patients could get some level of critical care. You can read more about this on the Wikipedia ICU page.
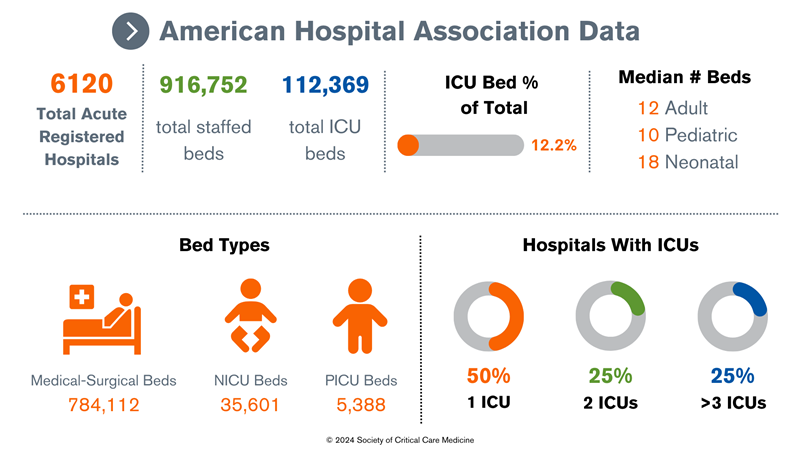
Data Snapshot: Icu Vs. Critical Care Beds Worldwide
Here’s a quick look at ICU and critical care bed counts in selected countries (data from 2022):
| Country | ICU Beds per 100,000 People | All Critical Care Beds per 100,000 People |
|---|---|---|
| United States | 34.7 | 49.2 |
| Germany | 29.2 | 40.5 |
| United Kingdom | 7.3 | 10.5 |
| India | 2.3 | 3.6 |
Notice that the number of critical care beds is always higher than ICU beds. This is because it includes HDU, CCU, and other specialty beds.
Practical Tips For Families And Patients
If a doctor says your loved one needs an ICU bed, ask:
- What makes the ICU necessary for them?
- Can their condition be managed in an HDU or other critical care unit?
- What equipment and staff are available in each unit?
- What are the visiting policies and infection risks?
If ICU beds are full, ask if another critical care bed is safe for your loved one’s condition. Doctors can explain the risks and benefits.
Non-obvious insight: Sometimes, patients do better outside the ICU once they are stable, as they can sleep better and have more family visits.
Another insight: ICU care is not always “better”—it is only better for those who truly need constant, advanced support.
Frequently Asked Questions
What Is The Main Difference Between An Icu Bed And A Critical Care Bed?
The main difference is that an ICU bed is always in the intensive care unit and has the highest level of monitoring, staffing, and life support equipment. A critical care bed can be in other high-level units like the HDU or CCU and may not have all the same equipment or staff.
Can A Hospital Have Critical Care Beds But No Icu Beds?
Yes. Some small hospitals or specialty centers may have critical care beds in the HDU or CCU but not a full ICU. However, they will transfer the sickest patients to a hospital with an ICU if needed.
Are Patients In An Hdu Getting Worse Care Than In The Icu?
No. Patients in the HDU are usually more stable and do not need full ICU care. The care is matched to their needs. Moving someone from the ICU to the HDU often means they are improving.
Why Are Icu Beds More Expensive Than Other Critical Care Beds?
ICU beds cost more because they need more staff, advanced equipment, and intensive monitoring. The cost covers specialized doctors, 24/7 nursing, and machines like ventilators and dialysis.
How Can Families Know If Their Loved One Should Be In The Icu Or Another Critical Care Bed?
Families should ask the care team about the patient’s condition, what organ support is needed, and what care is available in each unit. Doctors use guidelines and scoring systems to match the patient to the safest level of care.
When you understand the difference between ICU beds and critical care beds, you can make better choices and ask the right questions in a stressful time. This knowledge can help you advocate for the best possible care—without unnecessary worry or confusion.